Ibogaine
From Wikipedia, the free encyclopedia
 |
|
 |
|
|
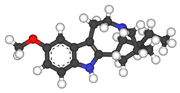
Ibogaine
|
|
| Systematic (IUPAC) name | |
| 12-Methoxyibogamine | |
| Identifiers | |
| CAS number | |
| ATC code | ? |
| PubChem | |
| ChemSpider | |
| Chemical data | |
| Formula | C20H26N2O |
| Mol. mass | 310.433 g/mol |
| SMILES | & |
| Physical data | |
| Melt. point | 152–153 °C (306–307 °F) |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | 2 hours |
| Excretion | ? |
| Therapeutic considerations | |
| Pregnancy cat. |
? |
| Legal status | |
| Routes | oral |
Ibogaine is a naturally occurring psychoactive compound found in a number of plants, principally in a member of the dogbane family known as iboga (Tabernanthe iboga). Ibogaine-containing preparations are used in medicinal and ritual purposes within African spiritual traditions of the Bwiti, who claim to have learned it from the Pygmy. In recent times, it has been identified as having anti-addictive properties. Ibogaine is an indole alkaloid that is obtained either by extraction from the iboga plant or by semi-synthesis from the precursor compound voacangine, another plant alkaloid. A full organic synthesis of ibogaine has been achieved but is too expensive and challenging to produce any commercially significant yield.
In the early 1960s, ibogaine was accidentally discovered to cause sudden and complete interruption of heroin addiction without withdrawal in a matter of hours. Since that time, it has been the subject of scientific investigation into its abilities to interrupt addictions to heroin, alcohol, and cocaine. Anecdotal reports also suggest that ibogaine may have potential to drive introspection that helps elucidate the psychological issues and behavior patterns that drive addictions or other problems. However, ibogaine therapy for drug addiction is the subject of some controversy. Due to its hallucinogenic properties, it has been placed in the strictest drug prohibition schedules in the United States and a handful of other countries. Canada and Mexico both allow ibogaine treatment clinics to operate and openly contribute to further understanding of the addictive process.
While ibogaine's prohibition has slowed scientific research into its anti-addictive properties, the use of ibogaine for drug treatment has grown in the form of a large worldwide medical subculture.[1] Ibogaine is now used by treatment clinics in 12 countries on six continents to treat addictions to heroin, alcohol, powder cocaine, crack cocaine, and methamphetamine, as well as to facilitate psychological introspection and spiritual exploration.
Contents |
[edit] Psychoactive effects
At doses of around 3–5 mg/kg of body weight, ibogaine has a mild stimulant effect. The high-dose ibogaine experience of 10 mg/kg or greater most commonly occurs as two distinct phases: the visual phase and the introspective phase.
The visual phase is characterized by open-eye visuals, closed-eye visuals, and dreamlike sequences. Objects may be seen as distorted, projecting tracers, or having moving colors or textures. With the eyes closed, extremely detailed and vivid geometric and fractal visions may be seen. Subjective reports often include a movie-like recollection of earlier life experiences as well as dreamlike sequences with symbolism of one's present or anticipated future. Other effects in the visionary phase may include laughing, sensations of euphoria or fear, and temporary short-term memory impairment. The visionary phase usually ends after one to four hours, after which the introspective phase begins.
The introspective phase is typically reported to bring elevated mood, a sense of calm and euphoria, and a distinct intellectual and emotional clarity. Subjects often report being able to accomplish deep emotional and intellectual introspection into psychological and emotional concerns. It is also during this period that opioid addicts first notice the absence of withdrawal cravings. The duration of the introspective phase is highly variable, usually lasting hours but sometimes lasting days.
[edit] Side effects and safety
One of the first noticeable effects of large-dose ibogaine ingestion is ataxia, a difficulty in coordinating muscle motion which makes standing and walking virtually impossible without assistance. Xerostomia (dry mouth), nausea, and vomiting may follow. These symptoms are long in duration, ranging from 4 to 24 hours in some cases. Ibogaine is sometimes administered by enema to help the subject avoid vomiting up the dose. Psychiatric medications are strongly contraindicated in ibogaine therapy due to adverse interactions. Some studies also suggest the possibility of adverse interaction with heart conditions. In one study of canine subjects, ibogaine was observed to increase sinus arrhythmia (the normal change in heart rate during respiration).[2] Ventricular ectopy has been observed in a minority of patients during ibogaine therapy.[3] It has been proposed that there is a theoretical risk of QT-interval prolongation following ibogaine administration.[4] This risk was further demonstrated by a case reported in the New England Journal of Medicine documenting prolonged QT interval and ventricular tachycardia after initial use. [5]
There are 12 documented fatalities that have been loosely associated with ibogaine ingestion.[6] Exact determinations of the cause of death have proven elusive due to the quasi-legal status of ibogaine and the unfamiliarity of medical professionals with this relatively rare substance. No autopsy to date has implicated ibogaine as the sole cause of death. Causes given range from significant pre-existing medical problems to the surreptitious consumption of other drugs in conjunction with ibogaine. Most legal and illegal psychoactive drugs are strongly contraindicated during or immediately after ibogaine treatment, which presents a risk in undersupervised or self-treating subjects.
[edit] Therapeutic uses
[edit] Treatment for opiate addiction
The most-studied long-term therapeutic effect is that ibogaine seems to catalyze partial or complete interruption of addiction to opioids. An integral effect is the alleviation of symptoms of opioid withdrawal. Research also suggests that ibogaine may be useful in treating dependence on other substances such as alcohol, methamphetamine, and nicotine and may affect compulsive behavioral patterns not involving substance abuse or chemical dependence.
Proponents of ibogaine treatment for drug addiction have established formal and informal clinics or self-help groups in Canada, Mexico, the Caribbean, Costa Rica, the Czech Republic, France, Slovenia, the Netherlands, Brazil, South Africa, the United Kingdom and New Zealand, where ibogaine is administered as an experimental drug. There also exist clandestine drug-treatment facilities in the countries where it is illegal. Although the full nature of ibogaine is still emerging, it appears that the most effective treatment paradigm involves visionary doses of ibogaine of 10–20 mg/kg, producing an interruption of opiate withdrawal and craving. Many users of ibogaine report experiencing visual phenomena during a waking dream state, such as instructive replays of life events that led to their addiction, while others report therapeutic shamanic visions that help them conquer the fears and negative emotions that might drive their addiction. It is proposed that intensive counseling and therapy during the interruption period following treatment is of significant value. Some patients require a second or third treatment session with ibogaine over the course of the next 12 to 18 months, as it will provide a greater efficacy in extinguishing the opiate addiction or other drug dependence syndrome. A minority of patients relapse completely into opiate addiction within days or weeks. A comprehensive article (Lotsof 1995) on the subject of ibogaine therapy detailing the procedure, effects and aftereffects is found in "Ibogaine in the Treatment of Chemical Dependence Disorders: Clinical Perspectives".[7] Ibogaine has also been reported in multiple small-study cohorts to reduce cravings for methamphetamine. [8]
[edit] Chronic pain management
In 1957, Jurg Schneider, a pharmacologist at CIBA, found that ibogaine potentiates morphine analgesia.[9] Further research was abandoned, and no additional data was ever published by Ciba researchers on ibogaine–opioid interactions. Almost 50 years later, Patrick Kroupa and Hattie Wells released the first treatment protocol for concomitant administration of ibogaine with opioids in human subjects, indicating ibogaine reduced tolerance to opioid drugs.[10] Kroupa et al. published their research in the Multidisciplinary Association for Psychedelic Studies Journal demonstrating that administration of low-"maintenance" doses of ibogaine HCl with opioids decreases tolerance.
[edit] Psychotherapy
Ibogaine has been used as an adjunct to psychotherapy by Claudio Naranjo, documented in his book The Healing Journey.[11]
[edit] Recreational use
Casual use of ibogaine in a social or entertainment context is nearly unknown due to its high cost, constrained availability, long duration of effects, and uncomfortable short-term side effects. In the clandestine markets, ibogaine is typically sought as a drug addiction treatment, for ritual spiritual purposes, or psychological introspection.
[edit] History
It is uncertain exactly how long iboga has been used in African spiritual practice, but its activity was first observed by French and Belgian explorers in the 19th century. The first botanical description of the Tabernanthe iboga plant was made in 1889. Ibogaine was first isolated from T. iboga in 1901 by Dybowski and Landrin[12] and independently by Haller and Heckel in the same year using T. iboga samples from Gabon. In the 1930s, ibogaine was sold in France in 8 mg tablets under the name "Lambarene". The total synthesis of ibogaine was accomplished by G. Büchi in 1966.[13] Since then, several further totally synthetic routes have been developed.[14] The use of ibogaine in treating substance use disorders in human subjects was first observed by Howard Lotsof in 1962, for which he was later awarded U.S. Patent 4,499,096 in 1985. In 1969, Claudio Naranjo was granted a French patent for the use of ibogaine in psychotherapy.
Ibogaine was placed in US Schedule 1 in 1967 as part of the US government's strong response to the upswing in popularity of psychedelic substances, though iboga itself was scarcely known at the time. Ibogaine's ability to attenuate opioid withdrawal confirmed in the rat was first published by Dzoljic et al. (1988).[15] Ibogaine's use in diminishing morphine self-administration in preclinical studies was shown by Glick et al. (1991)[16] and ibogaine's capacity to reduce cocaine self-administration in the rat was shown by Cappendijk et al. (1993).[17] Animal model support for ibogaine claims to treat alcohol dependence were established by Rezvani (1995).[18]
The name "Indra extract", in strict terms, refers to 44 kg of an iboga extract manufactured by an unnamed European industrial manufacturer in 1981. This stock was later purchased by Carl Waltenburg, who distributed it under the name "Indra extract". Waltenburg used this extract to treat heroin addicts in Christiania, Denmark, a squatter village where heroin addiction was widespread in 1982.[19] Indra extract was offered for sale over the Internet until 2006, when the Indra web presence disappeared. It is unclear whether the extracts currently sold as "Indra extract" are actually from Waltenburg's original stock, or whether any of that stock is even viable or in existence. Ibogaine and related indole compounds are susceptible to oxidation when exposed to oxygen[20], as opposed to their salt form, which is stable. The exact methods and quality of the original Indra extraction was never documented, so the real composition of the product remains uncertain.
Data demonstrating ibogaine's efficacy in attenuating opioid withdrawal in drug-dependent human subjects was published by Alper et al. (1999)[21] and Mash et al. (2000).[22]
In 1972, journalist Hunter S. Thompson accused democratic candidate Edmund Muskie of being addicted to ibogaine in a satirical piece. Many readers, and even other journalists, did not realize that Thompson was being facetious. The claim, of course, was completely unfounded, and Thompson himself is documented in the movie Gonzo: The Life and Work of Dr. Hunter S. Thompson discussing the self-fabricated joke of Muskie's alleged ibogaine use and his surprise that anyone actually believed the claim.
[edit] Formulations
Pure crystalline ibogaine hydrochloride is the most standardized formulation dosing and typically must be produced by the semi-synthesis from voacangine in commercial laboratories. In Bwiti religious ceremonies, the rootbark is pulverized and swallowed in large amounts to produce intense psychoactive effects. In Africa, iboga rootbark is sometimes chewed, which releases small amounts of ibogaine to produce a stimulant effect. Ibogaine is also available in a total alkaloid extract of the Tabernanthe iboga plant, which also contains all the other iboga alkaloids and thus has only about one-fifth the potency by weight as standardized ibogaine hydrochloride.[23]
Total alkaloid extracts of T. iboga are often loosely called "Indra extract". However, that name actually refers to a particular stock of total alkaloid extract produced in Europe in 1981. The fate of that original stock (as well as its original quality) is unknown.
[edit] Pharmacology
The pharmacology of ibogaine is quite complex, affecting many different neurotransmitter systems simultaneously.[24][25] Because of its fairly low potency at any of its target sites, ibogaine is used in doses anywhere from 5 mg/kg of body weight for a minor effect to 30 mg/kg in the cases of strong polysubstance addiction. It is unknown whether doses greater than 30 mg/kg in humans produce effects that are therapeutically beneficial, medically risky, or simply prolonged in duration. In animal neurotoxicity studies, there was no observable neurotoxicity of ibogaine at 25 mg/kg, but at 50mg/kg, one-third of the rats had developed patches of neurodegeneration, and at doses of 75mg/kg or above, all rats showed a characteristic pattern of degeneration of Purkinje neurons, mainly in the cerebellum.[26] While caution should be exercised when extrapolating animal studies to humans, these results suggest that neurotoxicity of ibogaine is likely to be minimal when ibogaine is used in the 10-20 mg/kg range typical of drug addiction interruption treatment regimes, and indeed death from the other pharmacological actions of the alkaloids is likely to occur by the time the dose is high enough to produce consistent neurotoxic changes.[27][28]
[edit] Pharmacodynamics
Among recent proposals for ibogaine mechanisms of action is activation of the glial cell line-derived neurotrophic factor (GDNF) pathway in the ventral tegmental area (VTA) of the brain. The work has principally been accomplished in preclinical ethanol research, where 40 mg/kg of ibogaine caused increases of RNA expression of GDNF in keeping with reduction of ethanol intake in the rat, absent neurotoxicity or cell death.[29]
Ibogaine is a noncompetitive antagonist at α3β4 nicotinic receptors, binding with moderate affinity.[30] Several other α3β4 antagonists are known, and some of these, such as bupropion (Wellbutrin or Zyban), and mecamylamine, have been used for treating nicotine addiction. This α3β4 antagonism correlates quite well with the observed effect of interrupting addiction. Co-administration of ibogaine with other α3β4 antagonists such as 18-MC, dextromethorphan or mecamylamine had a stronger anti-addictive effect than when it was administered alone.[31] Since α3β4 channels and NMDA channels are related to each other and their binding sites within the lumen bind a range of same ligands (e.g. DXM, PCP),[32] some older sources suggested that ibogaine's anti-addictive properties may be (partly) due to it being an NMDA receptor antagonist.[33] However, ligands, like 18-MC, selective for α3β4- vs. NMDA-channels showed no drop-off in activity.
It is suspected that ibogaine's actions on the opioid and glutamatergic systems are also involved in its anti-addictive effects. Persons treated with ibogaine report a cessation of opioid withdrawal signs generally within an hour of administration.
Ibogaine is a weak 5HT2A receptor agonist[34], and although it is unclear how significant this action is for the anti-addictive effects of ibogaine, it is likely to be important for the hallucinogenic effects.[35] Ibogaine is also a sigma2 receptor agonist.[36]
[edit] Metabolites
Ibogaine is metabolized in the human body by cytochrome P450 2D6, and the major metabolite is noribogaine (12-hydroxyibogamine). Noribogaine is most potent as a serotonin reuptake inhibitor and acts as a moderate κ- and weak µ-opioid receptor full agonist and therefore, also has an aspect of an opiate replacement similar to compounds like methadone. Both ibogaine and noribogaine have a plasma half-life of around two hours in the rat[37], although the half-life of noribogaine is slightly longer than the parent compound. It is proposed that ibogaine is deposited in fat and metabolized into noribogaine as it is released.[38] Noribogaine shows higher plasma levels than ibogaine and may therefore be detected for longer periods of time than ibogaine. Noribogaine is also more potent than ibogaine in rat drug discrimination assays when tested for the subjective effects of ibogaine.[39] Noribogaine differs from ibogaine in that it contains a hydroxy instead of a methoxy group at the 12 position.
[edit] Analogs
A synthetic derivative of ibogaine, 18-methoxycoronaridine (18-MC), is a selective α3β4 antagonist that was developed collaboratively by the neurologist Stanley D. Glick (Albany) and the chemist Martin E. Kuehne (Vermont).[40] This discovery was stimulated by earlier studies on other naturally occurring analogues of ibogaine such as coronaridine and voacangine that showed these compounds also have anti-addictive properties.[41][42]
[edit] Isomerism
Ibogaine has two separate chiral centers which means that there a four different stereoisomers of ibogaine. These four isomers are difficult to resolve.[43]
[edit] Research
An ibogaine research project was funded by the US National Institute on Drug Abuse in the early 1990s. The National Institute on Drug Abuse (NIDA) abandoned efforts to continue this project into clinical studies in 1995, citing other reports that suggested a risk of brain damage with extremely high doses and fatal heart arrhythmia in patients having a history of health problems, as well as inadequate funding for ibogaine development within their budget. However, NIDA funding for ibogaine research continues in indirect grants often cited in peer-reviewed ibogaine publications.
In addition, after years of work and a number of significant changes to the original protocol, on August 17, 2006, a MAPS-sponsored research team received "unconditional approval" from a Canadian Institutional Review Board (IRB) to proceed with a long-term observational case study that will examine changes in substance use in 20 consecutive people seeking ibogaine-based addiction treatment for opiate dependence at the Iboga Therapy House in Vancouver.
[edit] Legal status
Ibogaine and its salts were regulated by the U.S. Food and Drug Administration in 1967 pursuant to its enhanced authority to regulate stimulants, depressants, and hallucinogens granted by the 1965 Drug Abuse Control Amendments (DACA) to the Federal Food, Drug, and Cosmetic Act. In 1970, with the passage of the Controlled Substances Act, it was classified as a Schedule I-controlled substance in the United States, along with other psychedelics such as LSD and mescaline. Since that time, several other countries, including Sweden, Denmark, Belgium, and Switzerland, have also banned the sale and possession of ibogaine. Although illegal, ibogaine has been used by hundreds of drug addicts in the United States and abroad. Howard Lotsof, a pioneer in bringing awareness to ibogaine's success in helping hardcore drug dependents to quit their addiction, and others have been offering willing persons the treatment. In the Czech Republic and Slovenia, taking advantage of less prohibitive legal systems, ibogaine has been applied to people coming from the U.S. and other countries seeking a safe haven.
[edit] Canada
Ibogaine is not scheduled as an illegal drug in Canada. (http://laws.justice.gc.ca/en/ShowFullDoc/cs/C-38.8///en)
[edit] Sweden
In early 2006, a non-profit foundation addressing the issue of providing ibogaine for the purpose of addiction interruption within established drug treatment care was formed in Sweden.[44]
[edit] See also
[edit] References
- ^ K.R. Alper, H.S. Lotsof, C.D. Kaplan (2008). "The Ibogaine Medical Subculture". J. Ethnopharmacology 115: 9–24. doi:. http://www.ibogaine.org/subculture.html. Retrieved on 2008-02-22.
- ^ http://www.puzzlepiece.org/ibogaine/literature/gershon1962.pdf
- ^ Dora Weiner Foundation Conferences: 2004, Reports and Exhibits - AATOD and HRC
- ^ Fatalities after taking ibogaine in addiction trea...[Med Hypotheses. 2006] - PubMed Result
- ^ Hoelen DW, Spiering W, Valk GD Long-QT syndrome induced by the antiaddiction drug ibogaine. N Engl J Med. 2009 Jan 15;360(3):308-9. PMID 19144953
- ^ Ibogaine & Eboga (Related) Recorded Fatalities
- ^ H.S. Lotsof (1995). Ibogaine in the Treatment of Chemical Dependence Disorders: Clinical Perspectives (Originally published in MAPS Bulletin (1995) V(3):19-26)
- ^ AJ Giannini.Drugs of Abuse--Second Edition. Los Angeles, Practice Management Information Corp.,1997.
- ^ Jurg Schneider (assignee: Ciba Pharmaceuticals), Tabernanthine, Ibogaine Containing Analgesic Compositions. US Patent No. 2,817,623 (1957) (pdf)
- ^ Patrick K. Kroupa, Hattie Wells (2005): Ibogaine in the 21st Century. Multidisciplinary Association for Psychedelic Studies. Volume XV, Number 1: 21-25 (pdf)
- ^ C. Naranjo. The Healing Journey. Chapter V, Ibogaine: Fantasy and Reality, 197-231, Pantheon Books, Div. Random House,ISBN 0394488261, New York (1973)
- ^ J. Dybowski, E. Landrin (1901). "PLANT CHEMISTRY. Concerning Iboga, its excitement-producing properties, its composition, and the new alkaloid it contains, ibogaine". C. R. Acad. Sci. 133: 748. http://ibogaine.desk.nl/dybowski.html. Retrieved on 2006-06-23.
- ^ G. Büchi, D.L. Coffen, Karoly Kocsis, P.E. Sonnet, and Frederick E. Ziegler (1966). "The Total Synthesis of Iboga Alkaloids" (pdf). J. Am. Chem. Soc. 88 (13): 3099–3109. doi:. http://pubs.acs.org/cgi-bin/abstract.cgi/jacsat/1966/88/i13/f-pdf/f_ja00965a039.pdf. Retrieved on 2006-06-23.
- ^ C. Frauenfelder (1999) Doctoral Thesis, page 24 (pdf)
- ^ E.D. Dzoljic et al. (1988): "Effect of ibogaine on naloxone-precipitated withdrawal syndrome in chronic morphine-dependent rats" Arch. Int. Pharmacodyn. Ther. 294, 64-70
- ^ Glick S.D., Rossman K., Steindorf S., Maisonneuve I.M., and Carlson J.N. (1991). "Effects and aftereffects of ibogaine on morphine self-administration in rats". Eur. J. Pharmacol 195 (3): 341–345. doi:. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=1868880&dopt=Citation. Retrieved on 2006-06-24.
- ^ Cappendijk SLT, Dzoljic MR (1993). "Inhibitory effects of ibogaine on cocaine self-administration in rats". European Journal of Pharmacology 241: 261–265. doi:. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?db=pubmed&cmd=Retrieve&dopt=Abstract&list_uids=8243561&query_hl=5&itool=pubmed_docsum. Retrieved on 2006-06-25.
- ^ Rezvani, A., Overstreet D., and Lee, Y. (1995). "Attenuation of alcohol intake by ibogaine in three strains of alcohol preferring rats.". Pharmacology, Biochemistry, and Behaviour 52: 615–620. doi:. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?db=pubmed&cmd=Retrieve&dopt=Abstract&list_uids=8545483&query_hl=1&itool=pubmed_docsum. Retrieved on 2006-06-25.
- ^ A Contemporary History of Ibogaine in the United States and Europe
- ^ a)Taylor WI (1965): "The Iboga and Voacanga Alkaloids" (Journal?), Pages 203, 207 and 208. Oxidation products: peroxides; indolenine, iboquine and iboluteine. pdf b) Also compare PMID 16959135
- ^ Alper et al. (1999) "Treatment of acute opioid withdrawal with ibogaine." Am J Addict. 1999 Summer;8(3):234-42 (pdf)
- ^ D.C. Mash, et al. (2000). Ibogaine: Complex Pharmacokinetics, Concerns for Safety, and Preliminary Efficacy Measures (pdf). Neurobiological Mechanisms of Drugs of Abuse Volume 914 of the Annals of the New York Academy of Sciences, September 2000.
- ^ Jenks CW (2002)
- ^ P. Popik, P. Skolnick (1998). Pharmacology of Ibogaine and Ibogaine-Related Alkaloids. The Alkaloids 52, Chapter 3, 197-231, Academic Press, Editor: G.A. Cordell
- ^ K.R. Alper (2001). Ibogaine: A Review. The Alkaloids 56, 1-38, Academic Press (pdf)
- ^ Xu Z, Chang LW, Slikker W Jr, Ali SF, Rountree RL, Scallet AC. A dose-response study of ibogaine-induced neuropathology in the rat cerebellum. Toxicological Sciences. 2000 Sep;57(1):95-101. PMID 10966515
- ^ Kontrimaviciūte V, Mathieu O, Mathieu-Daudé JC, Vainauskas P, Casper T, Baccino E, Bressolle FM. Distribution of ibogaine and noribogaine in a man following a poisoning involving root bark of the Tabernanthe iboga shrub. Journal of Analytical Toxicology. 2006 Sep;30(7):434-40. PMID 16959135
- ^ Maciulaitis R, Kontrimaviciute V, Bressolle F, Briedis V. Ibogaine, an anti-addictive drug: pharmacology and time to go further in development. A narrative review. Human and Experimental Toxicology. 2008 Mar;27(3):181-94. PMID 18650249
- ^ He, Dao-Yao et al. (2005): "Glial Cell Line-Derived Neurotrophic Factor Mediates the Desirable Actions of the Anti-Addiction Drug Ibogaine against Alcohol Consumption." Journal of Neuroscience, 25(3), pp. 619–628. Fulltext
- ^ Glick SD, Maisonneuve IM, Kitchen BA, Fleck MW. Antagonism of alpha 3 beta 4 nicotinic receptors as a strategy to reduce opioid and stimulant self-administration. European Journal of Pharmacology. 2002 Mar 1;438(1-2):99-105.
- ^ Glick SD, Maisonneuve IM, Kitchen BA. Modulation of nicotine self-administration in rats by combination therapy with agents blocking alpha 3 beta 4 nicotinic receptors. European Journal of Pharmacology. 2002 Jul 19;448(2-3):185-91.
- ^ Fryer JD, Lukas RJ. Noncompetitive functional inhibition at diverse, human nicotinic acetylcholine receptor subtypes by bupropion, phencyclidine, and ibogaine. Journal of Pharmacology and Experimental Therapeutics. 1999 Jan;288(1):88-92.
- ^ Popik P, Layer RT, Skolnick P (1994): "The putative anti-addictive drug ibogaine is a competitive inhibitor of [3H]MK-801 binding to the NMDA receptor complex." Psychopharmacology (Berl), 114(4), 672-4. Abstract
- ^ Glick SD et al. (1999): "(±)-18-Methoxycoronaridine: A Novel Iboga Alkaloid Congener Having Potential Anti-Addictive Efficacy." CNS Drug Reviews, Vol. 5, No. 1, pp. 27-42, see p. 35. Fulltext
- ^ Helsley S, Fiorella D, Rabin RA, Winter JC. Behavioral and biochemical evidence for a nonessential 5-HT2A component of the ibogaine-induced discriminative stimulus. Pharmacology, Biochemistry and Behaviour. 1998 Feb;59(2):419-25.
- ^ Mach RH, Smith CR, Childers SR (1995): "Ibogaine possesses a selective affinity for sigma 2 receptors." Life Sciences, 57(4), PL57-62. Abstract
- ^ "In Vivo Neurobiological Effects of Ibogaine and Its O-Desmethyl Metabolite, 12-Hydroxyibogamine (Noribogaine), in Rats -- Baumann et al. 297 (2): 531 -- Journal of Pharmacology And Experimental Therapeutics". http://jpet.aspetjournals.org/cgi/content/full/297/2/531.
- ^ Lindsay B. Hough, Sandra M. Pearl and Stanley D. Glick. Tissue Distribution of Ibogaine After Intraperitoneal and Subscutaneous Administration. Life Sciences 58(7) (1996): 119–122. Abstract
- ^ C Zubaran MD, M Shoaib Ph.D, IP Stolerman Ph.D, J Pablo MS and DC Mash Ph.D. Noribogaine Generalization to the Ibogaine Stimulus: Correlation with Noribogaine Concentration in Rat Brain. Neuropsychopharmacology (1999) 21 119-126.10.1038/sj.npp.1395327. [1]
- ^ Christopher J. Pace, Stanley D. Glick, Isabelle M. Maisonneuve, Li-Wen Heb, Patrick A. Jokiel, Martin E. Kuehne, Mark W. Fleck. Novel iboga alkaloid congeners block nicotinic receptors and reduce drug self-administration. European Journal of Pharmacology 492 (2004): 159–167.
- ^ Glick SD, Kuehne ME, Raucci J, Wilson TE, Larson D, Keller RW Jr, Carlson JN. Effects of iboga alkaloids on morphine and cocaine self-administration in rats: relationship to tremorigenic effects and to effects on dopamine release in nucleus accumbens and striatum. Brain Research. 1994 Sep 19;657(1-2):14-22. PMID 7820611
- ^ Tsing Hua. Antiaddictive indole alkaloids in Ervatamia yunnanensis and their bioactivity. Academic Journal of Second Military Medical University. January 28, 2006.
- ^ Shulgin & Shulgin (1997), TiHKAL, p. 487.
- ^ Stiftelsen Iboga´s web site
[edit] External links
- Erowid Ibogaine Vault
- Ibogaine Dossier
- Ibogaine UK
- MindVox Ibogaine Site and Forums
- The Ibogaine Research Project
- Ibogaine Patients' Bill of Rights
- Ibogaine & Addiction
- Ibogaine on CBS Channel 5; February, 2005
- Ten years of therapy in one night
- Ibogaine: A Novel Anti-Addictive Compound - A Comprehensive Literature Review
- Ibogaine article from Utne Reader
[edit] Further reading
- Daniel Pinchbeck writes of his own experience with ibogaine (among other psychoactives) in Breaking Open the Head.
- Ibogaine: Rite Of Passage is a documentary film about the use of ibogaine in Bwiti tradition and addiction medicine.
|
|||||


